While we try to keep things accurate, this content is part of an ongoing experiment and may not always be reliable.
Please double-check important details — we’re not responsible for how the information is used.
Bacteria
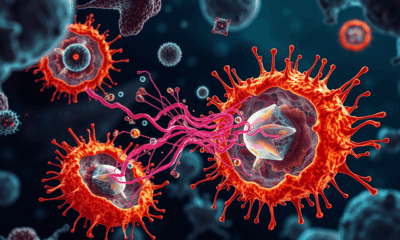
Predicting Antibiotic Resistance with AI
An AI model trained on large amounts of genetic data can predict whether bacteria will become antibiotic-resistant. The new study shows that antibiotic resistance is more easily transmitted between genetically similar bacteria and mainly occurs in wastewater treatment plants and inside the human body.

Allergy
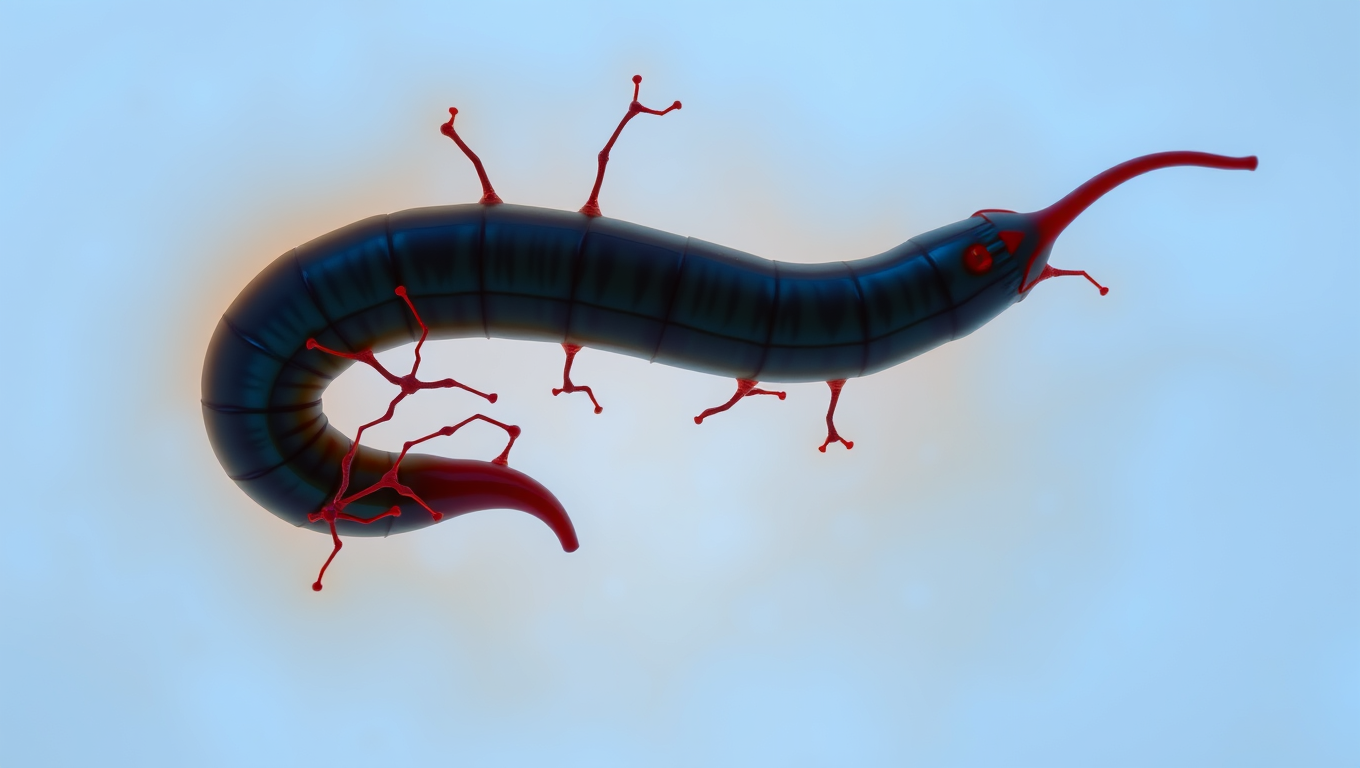
“The Silent Invader: How a Parasitic Worm Evades Detection and What it Can Teach Us About Pain Relief”
Scientists have discovered a parasite that can sneak into your skin without you feeling a thing. The worm, Schistosoma mansoni, has evolved a way to switch off the body’s pain and itch signals, letting it invade undetected. By blocking certain nerve pathways, it avoids triggering the immune system’s alarms. This stealth tactic not only helps the worm survive, but could inspire new kinds of pain treatments and even preventative creams to protect people from infection.
Bacteria
Unlocking the Secrets of Mars: Cosmic Rays Reveal Hidden Potential for Life
Cosmic rays from deep space might be the secret energy source that allows life to exist underground on Mars and icy moons like Enceladus and Europa. New research reveals that when these rays interact with water or ice below the surface, they release energy-carrying electrons that could feed microscopic life, a process known as radiolysis. This breakthrough suggests that life doesn’t need sunlight or heat, just some buried water and radiation.
Alternative Medicine
Cleaning Up the Water, Cooling Down the Risks: A New Approach to Safer Romaine Lettuce
Romaine lettuce has a long history of E. coli outbreaks, but scientists are zeroing in on why. A new study reveals that the way lettuce is irrigated—and how it’s kept cool afterward—can make all the difference. Spraying leaves with untreated surface water is a major risk factor, while switching to drip or furrow irrigation cuts contamination dramatically. Add in better cold storage from harvest to delivery, and the odds of an outbreak plummet. The research offers a clear, science-backed path to safer salads—one that combines smarter farming with better logistics.
-

 Detectors1 year ago
Detectors1 year agoA New Horizon for Vision: How Gold Nanoparticles May Restore People’s Sight
-

 Cancer1 year ago
Cancer1 year agoRevolutionizing Quantum Communication: Direct Connections Between Multiple Processors
-

 Earth & Climate1 year ago
Earth & Climate1 year agoRetiring Abroad Can Be Lonely Business
-

 Albert Einstein1 year ago
Albert Einstein1 year agoHarnessing Water Waves: A Breakthrough in Controlling Floating Objects
-

 Earth & Climate1 year ago
Earth & Climate1 year agoHousehold Electricity Three Times More Expensive Than Upcoming ‘Eco-Friendly’ Aviation E-Fuels, Study Reveals
-

 Chemistry1 year ago
Chemistry1 year ago“Unveiling Hidden Patterns: A New Twist on Interference Phenomena”
-

 Diseases and Conditions1 year ago
Diseases and Conditions1 year agoReducing Falls Among Elderly Women with Polypharmacy through Exercise Intervention
-

 Earth & Climate1 year ago
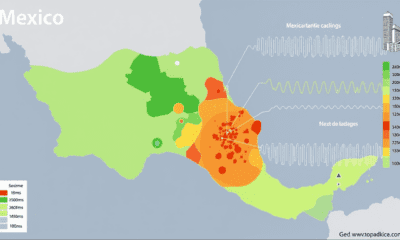
Earth & Climate1 year agoPredicting Damage from Local Earthquakes in Mexico City